The rollout of COVID-19 vaccines has been a critical development in the global fight against the pandemic. A growing body of research indicates that these vaccines not only reduce the incidence of infection but also significantly decrease all-cause mortality among vaccinated individuals compared to those who are unvaccinated.
- The accumulation of evidence solidly affirms that COVID-19 vaccines not only directly save lives by preventing virus-specific deaths but also play a crucial role in reducing all-cause mortality among vaccinated populations.
- While claims about COVID-19 vaccines being associated with increased mortality have circulated, they are often based on misinterpretation of data, anecdotal evidence, or preliminary research that does not stand up to rigorous scientific scrutiny.
- The consensus among health authorities and scientific community is that COVID-19 vaccines are a critical tool in reducing mortality and severe illness from the virus, with the benefits significantly outweighing the risks.
This blog outlines the key evidence supporting the impact of COVID-19 vaccines on reducing all-cause mortality and addresses some misinformation about the topic.
Direct effect – Prevention of COVID-19 deaths
Research across various COVID-19 vaccines, including those developed by Pfizer-BioNTech, Moderna, AstraZeneca, and Johnson & Johnson, has consistently demonstrated their effectiveness in averting deaths attributable to the virus. Clinical trials and real-world effectiveness studies have shown that these vaccines substantially lower the risk of severe disease, hospitalisation, and mortality due to COVID-19, particularly among high-risk groups such as older adults and individuals with underlying health conditions (Polack et al., 2020; Baden et al., 2021; Voysey et al., 2021).
Indirect effects – Reduction in all-cause mortality
Beyond preventing deaths directly attributed to COVID-19, research indicates that vaccination is associated with a reduction in all-cause mortality. This means that vaccinated individuals have a lower risk of dying from any cause compared to their unvaccinated counterparts during similar time periods. This effect is likely due to multiple factors:
- Reduction in healthcare system burden: With fewer severe cases of COVID-19, the pressure on healthcare systems is alleviated, ensuring better availability of care for both COVID-19 and non-COVID-19-related health issues, which may contribute to lower mortality rates from various causes (Lopez Bernal et al., 2021).
- Prevention of long-term health effects: COVID-19 can lead to persistent health complications, known as "Long COVID," which might increase mortality risk. Vaccination lowers the likelihood of Long COVID (Catala et al., 2024, Razzaghi et al., 2024) by either preventing the initial infection or mitigating its severity.
Population-Level studies
Evidence at the population level further corroborates the reduction in all-cause mortality associated with vaccination. Studies comparing mortality rates in populations with high vaccination coverage to those with lower levels of vaccination have consistently found reduced all-cause mortality rates in the more highly vaccinated groups, even after adjusting for factors such as age, sex, socioeconomic status, and pre-existing health conditions. This suggests a significant protective effect of vaccination on overall mortality (Palinkas & Sandor, 2022).
The global analysis of all-cause mortality and COVID-19 vaccination coverage by Mendoza-Cano et al. (2023) showed lower levels of all-cause mortality in countries with high vaccination coverage across 2020 and 2021. In the yellow and green world maps, countries with the lowest rates of excess death from all causes (lighter yellow colours) are the countries with the highest number of COVID-19 vaccines given (darkest green colour).
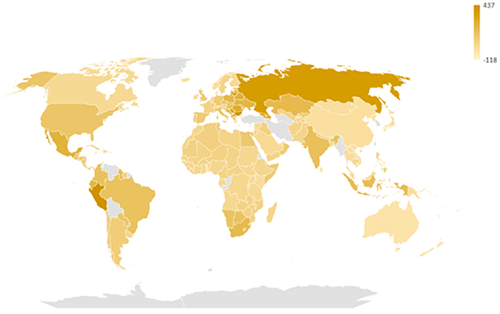
All-cause excess mortality rate (per 100,000) from 2020 to 2021 in the 178 analysed countries. Image source: Mendoza-Cano et al. (2023).
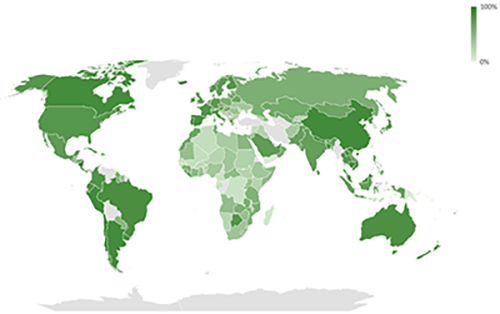
COVID-19 vaccination coverage until March 2023 in the 178 countries analysed. Image source: Mendoza-Cano et al. (2023).
The importance of age & age stratification
The practice of age stratification, or analysing data based on different age groups, is crucial in understanding mortality rates because it provides insights into which segments of the population are most at risk of death from various causes. Also, population trends change over time. In N.Z. and many other countries, the population is aging, each year more people enter the older age group.
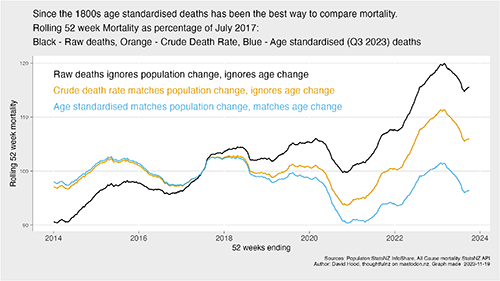
Graphs showing differences in rates of death when analysed as raw deaths, crude rates, and age standardised rates. Image source: David Hood, @Thoughtfulnz, https://twitter.com/Thoughtfulnz/status/1755890033083716074/photo/1
Age stratification in mortality analysis was recognised as vital as early as the 19th century with the work of life insurance companies and public health officials, who observed that mortality rates varied significantly with age, for example older people are usually more likely to die. By the mid-20th century, with advances in epidemiology and biostatistics, age stratification became a standard practice in analysing and reporting mortality data, helping to illuminate life expectancy trends, the impact of diseases on different age groups, and the effectiveness of health policies. This method is particularly important when dealing with diseases like COVID-19, where age is a strong factor in the likelihood of severe outcomes and death.
Without age stratification, findings could be misleading, masking the true impact of diseases on specific age groups. This can lead to inadequate health policies that fail to protect the most vulnerable populations. For a deeper understanding, visit these webpages: Epidemiology for Specialists and How does age standardization make health metrics comparable.
If you ever see people reporting on deaths following vaccination, ensure that they are reporting on rates that are age stratified.
Claims to the contrary
Misinterpretation of vaccine safety data
Some claims of increased mortality associated with COVID-19 vaccines stem from misinterpretations of Vaccine Adverse Event Reporting System (VAERS) data in the United States or similar reporting systems elsewhere. VAERS, for example, is an early warning system designed to detect possible safety issues with U.S. vaccines by collecting reports of adverse events following vaccination. However, reports to VAERS of death following vaccination do not automatically imply that the vaccine caused the death. The system accepts all reports without determining causality, which requires further investigation. Misinterpretation of these reports can lead to unfounded claims about vaccines increasing mortality. Read more about What VAERS is (and isn't).
 VAERS allows for the collection and analysis of information about adverse events (possible side effects) that could be associated with vaccines. Because the system is based on self-reporting, it is open to not only a wide range of genuine health concerns but also to erroneous, frivolous, or even joke submissions.
VAERS allows for the collection and analysis of information about adverse events (possible side effects) that could be associated with vaccines. Because the system is based on self-reporting, it is open to not only a wide range of genuine health concerns but also to erroneous, frivolous, or even joke submissions.
An example of such a non-serious submission was a report where an individual claimed to have turned into the Incredible Hulk after receiving a vaccine. Of course, this report was not a legitimate account of a vaccine side effect but rather a clear instance of misuse of the reporting system. VAERS is a valuable tool for public health researchers, and while it contains a vast amount of genuine data, it's important for the data to be carefully reviewed by medical experts to assess the validity and causality of reported adverse events. Such a review process typically excludes reports that are clearly false or implausible, such as someone transforming into a fictional character.
While the claim of a hulking would have been dismissed quickly by those responsible for reviewing VAERS reports, it serves as a reminder of the importance of critical analysis when interpreting data from open self-reporting systems. It's a testament to the openness and transparency of the VAERS system, but it also highlights the challenges in ensuring the accuracy and reliability of the data collected.
Image source: Bob Jagendorf, CC BY 2.0, via Wikimedia Commons
Anecdotal reports and case studies
Social media and some news outlets have highlighted anecdotal reports or isolated case studies of deaths occurring after COVID-19 vaccination. While each case warrants thorough investigation, these individual reports do not constitute scientific evidence that vaccines are causing increased mortality rates. Often, subsequent investigations by health authorities find that these deaths are unrelated to vaccination, stemming from underlying health conditions or other factors.
Disinformation
In late 2023 a New Zealand computer programmer named Barry Young working for Health New Zealand stole individual level health records related to CVOID-19 vaccination and gave them to U.S. tech entrepreneur Steve Kirsch. The data was ‘analysed’ and those involved claimed that it showed increased mortality following COVID-19 vaccines.
In fact, the stolen data showed the opposite, consistent with all other observations.
New Zealand is an excellent country to examine COVID-19 mortality and COVID-19 vaccines as it is one of only a few places that remained largely free of the virus until most of the population had been vaccinated. Not only was all-cause mortality lower that would normally have been predicted but the country experienced one of the lowest death rates from COVID-19. This is inconsistent with the claims on social media made by Young and Kirsch and supported by evidence from other countries such as Australia, Cyprus, Italy, and the U.S.
However, we didn't have clear numbers on how much this helped overall health. To help figure this out, researchers used a detailed computer model that considered different levels of vaccination in various age and ethnic groups. This model also took into account new factors like the introduction of antiviral drugs and changes in hospital data.
The findings were used to guide the N.Z. government's decisions in 2022 and 2023. By comparing different ‘what-if’ scenarios, the research suggested that vaccinations prevented about 6,650 deaths and stopped 45,100 hospital visits in an 18-month period. The number of lives saved might be even higher if we consider the effects of antiviral drugs. The study also highlighted that indigenous Māori had lower vaccination rates than Europeans, and if the rates were equal, up to 26% of Māori deaths might have been avoided. The takeaway? Vaccines significantly cut down health problems in N.Z. and making sure everyone has equal access to vaccines should be a priority.
Another example of disinformation involved Tiffany Dover, a nurse at CHI Memorial Hospital in Chattanooga, Tennessee, who experienced a fainting episode after receiving the COVID-19 vaccine during a live broadcast. This incident was used by some social media users to fuel false claims about the safety of the vaccine and her subsequent death. However, it was confirmed by the hospital and reported by Reuters that Dover is alive and well. The fainting episode was attributed to her known medical condition that often causes her to faint when experiencing pain, known as an overactive vagal response. This condition can be triggered by various stimuli, including pain from a vaccine injection.
Despite the hospital's confirmation and a video, they posted showing Dover after the incident, misinformation continued to spread online. Fact-checking organisations like PolitiFact and FactCheck.org have debunked the false claims about Dover's death. They have also explained that fainting can occur after any kind of vaccine and is not necessarily related to the vaccine itself but rather to the process of vaccination.
It's important to rely on verified sources and statements from official organisations or individuals directly involved in such incidents when confronting claims that circulate on social media. For further details, check out these "Search results".
Official statements and reviews
Health authorities worldwide, including the World Health Organization (WHO), the U.S. Centers for Disease Control and Prevention (CDC), the European Medicines Agency (EMA) and others, have conducted ongoing safety monitoring and comprehensive reviews of COVID-19 vaccines. These organisations have consistently concluded that the benefits of vaccination in preventing COVID-19 infection and its severe outcomes far outweigh any potential risks. Reports of adverse events, including deaths, are thoroughly investigated, with findings reinforcing the vaccines' safety profile. Read the International Coalition of Medicines Regulatory Authorities ICMRA statement on the safety of COVID-19 vaccines and the WHO Statement – COVID-19 vaccines saved at least 1.4 million lives in the European Region.
References
- Baden LR, El Sahly HM, Essink B, Kotloff K, Frey S, Novak R, et al. Efficacy and safety of the mRNA-1273 SARS-CoV-2 vaccine. N Engl J Med. 2020;384(5):403-16.
- Baker TB, Bolt DM, Smith SS, Piasecki TM, Conner KL, Bernstein SL, et al. The relationship of COVID-19 vaccination with mortality among 86,732 hospitalized patients: Subpopulations, patient factors, and changes over time. J Gen Intern Med. 2023;38(5):1248-55.
- Català M, Mercadé-Besora N, Kolde R, Trinh NTH, Roel E, Burn E, et al. The effectiveness of COVID-19 vaccines to prevent long COVID symptoms: Staggered cohort study of data from the UK, Spain, and Estonia. Lancet Respir Med. 2024.
- Cianci R, Franza L, Pignataro G, Massaro MG, Rio P, Tota A, et al. Effect of COVID-19 vaccination on the in-hospital prognosis of patients admitted during Delta and Omicron waves in Italy. Vaccines. 2023;11(2):373.
- Datta S, Vattiato G, Maclaren OJ, Hua N, Sporle A, Plank MJ. The impact of Covid-19 vaccination in Aotearoa New Zealand: A modelling study. Vaccine. Forthcoming 2024.
- Hoxha I, Agahi R, Bimbashi A, Aliu M, Raka L, Bajraktari I, et al. Higher COVID-19 vaccination rates are associated with lower COVID-19 mortality: A global analysis. Vaccines. 2023;11(1):74.
- Liu B, Stepien S, Dobbins T, Gidding H, Henry D, Korda R, et al. Effectiveness of COVID-19 vaccination against COVID-19 specific and all-cause mortality in older Australians: A population based study. Lancet Reg Health West Pac. 2023;40.
- Lopez Bernal J, Andrews N, Gower C, Gallagher E, Simmons R, Thelwall S, et al. Effectiveness of Covid-19 vaccines against the B.1.617.2 (Delta) variant. N Engl J Med. 2021;385(7):585-94.
- Lytras T, Athanasiadou M, Demetriou A, Stylianou D, Heraclides A, Kalakouta O. Lack of association between vaccination rates and excess mortality in Cyprus during the COVID-19 pandemic. Vaccine. 2023;41(18):2941-6.
- Mendoza-Cano O, Trujillo X, Huerta M, Ríos-Silva M, Guzmán-Esquivel J, Lugo-Radillo A, et al. Assessing the influence of COVID-19 vaccination coverage on excess mortality across 178 countries: A cross-sectional study. Vaccines. 2023;11(8):1294.
- Pálinkás A, Sándor J. Effectiveness of COVID-19 vaccination in Preventing all-cause mortality among adults during the third wave of the epidemic in Hungary: Nationwide retrospective cohort study. Vaccines. 2022;10(7):1009.
- Polack FP, Thomas SJ, Kitchin N, Absalon J, Gurtman A, Lockhart S, et al. Safety and efficacy of the BNT162b2 mRNA Covid-19 vaccine. N Engl J Med. 2020;383(27):2603-15.
- Razzaghi H, Forrest CB, Hirabayashi K, Wu Q, Allen A, Rao S, et al. Vaccine effectiveness against long COVID in children. Pediatrics. Forthcoming 2024.
- Shimabukuro TT, Nguyen M, Martin D, DeStefano F. Safety monitoring in the Vaccine Adverse Event Reporting System (VAERS). Vaccine. 2015;33(36):4398-405.
- Voysey M, Clemens SAC, Madhi SA, Weckx LY, Folegatti PM, Aley PK, et al. Safety and efficacy of the ChAdOx1 nCoV-19 vaccine (AZD1222) against SARS-CoV-2: An interim analysis of four randomised controlled trials in Brazil, South Africa, and the UK. Lancet. 2021;397(10269):99-111.
Updated: 22 February 2024
